| Table of Contents |  |
|
Case Report
| ||||||
| Squamous cell carcinoma in bladder secondary to Schistosoma haematobium infection | ||||||
| Ertugrul Gazi Ozbey | ||||||
|
Nyala Sudan Turkey Training and Research Hospital, Urology Department. Nyala-Darfur-Sudan.
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Ozbey EG. Squamous cell carcinoma in bladder secondary to Schistosoma haematobium infection. Edorium J Infect Dis 2015;2:7–10. |
|
Abstract
|
|
Introduction:
Despite the fact that urothelial carcinoma is the most common bladder tumor about 15% of bladder cancers have differentiated tumor types. Squamous cell carcinomas, which is one of these rare tumor types, are seen in 5% of schistosomiasis cases caused by infestation of Schistosoma haematobium parasitic worms where the disease is endemic.
Case Report: We would like to discuss a case that came to our clinic for a bladder tumor in a relatively young age and diagnosed with Schistosoma related squamous cell carcinoma by pathology department after she was treated with transurethral resection (TUR) of tumor with the help of previously published studies found in literature. Conclusion: Squamous cell carcinomas, which are rarely seen in bladder tumors, can also be caused by Schistosoma infections. | |
|
Keywords:
Bladder, Schistosoma haematobium, Squamous cell carcinoma
| |
|
Introduction
| ||||||
|
Bladder tumors are the second most common urological tumor type after prostate tumors. They are the fourth most common cancer type in males and eighth most common cancer in females [1]. Histopathologically, about 90% of tumors are transitional cell carcinomas (TCC), 5–7% are squamous cell carcinomas, 1–2% are adenocarcinomas and the rest 1–2% are undifferentiated carcinoma and mixed type tumors. Rare bladder epithelium tumors include villous adenoma, carcinoid tumors, carcinosarcoma and melanoma. In addition, non-epithelial tumors such as pheochromocytoma, lymphoma, choriocarcinoma and mesenchymal tumors might also be seen in bladder, even though those cases are quite rare. In Western countries, transient cell carcinomas are quite common due to tobacco use and occupational risk factors. For example, 92–99% of newly diagnosed cases in North America, Europe and Australia are transient cell carcinomas meanwhile this rate is 70–80% in Southwestern Asia and in some parts of Africa, those tumors are diagnosed in lower than 50% of cases have this histological type [2]. Squamous cell carcinomas in bladder are often linked to Schistosoma haematobium infections as a result of many studies on this subject. This parasite is endemic in 75 countries and concentrated especially in the countries within Middle East and some parts of Africa, with about 60% of total population of Egypt under direct risk for infection [3]. The bladder cancers linked with parasitic infections mainly affect men due to their tendency to work in rural and agricultural areas [4]. | ||||||
|
Case Report
| ||||||
|
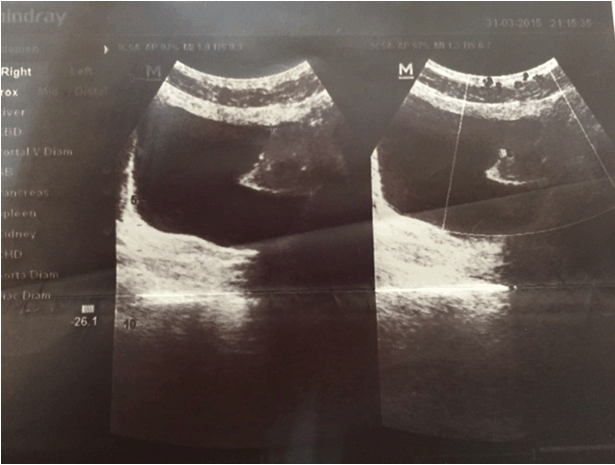
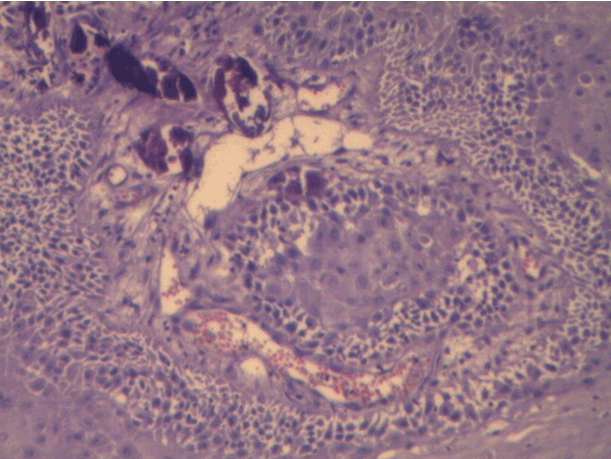
A 25-year-old male presented to our clinic with macroscopic hematuria complaint. After reviewing urinary system ultrasonography (USG) results, there was a 5-cm polypoid tumoral mass that almost completely filled the left wall of bladder. No pathology of upper urinary tract was detected in USG (Figure 1). Laboratory results of the patient were within normal range. Cystoscopy showed a solid calcified tumor-like lesion that completely covered left anterior wall surface. Lesion was resected using transurethral resection (TUR) technique. Bladder was mobile during bimanual examination. Patient made a full recovery without complications and was discharged. Pathology report of the resected mass during TUR came as verrucous type good differentiated keratinized squamous cell carcinoma. The report also said that there was lamina propria and muscle tissue invasion and calcified structures were consistent with Schistosoma eggs (Figure 2). After TUR-MT, a complete abdomen and thorax CT scans were ordered. The results were normal. Patient was planned with cystoprostatectomy and urinary diversion as a standard approach in invasive bladder tumors. | ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
About 90–95% of bladder tumors are from urothelium tissues. Moreover, 90% of these tumors are transitional epithelium cell carcinomas which are papillary tumors that grow towards lumen [2]. Rare epithelial tumors such as adenocarcinoma and squamous cell carcinomas can be seen together or apart on their own. Bladder adenocarcinomas can be urachus or bladder related or metastatic lesions. Adenocarcinomas found in bladder dome are mainly thought to arise from urachus. One of the common properties of these two types of rare bladder tumors with small cell carcinoma of bladder is that their prognosis is worse than transitional epithelium cell carcinoma. Those tumors are usually already in a high stage at the time of diagnosis and have low survival rates despite principally aggressive treatment. According to the World Health Organization (WHO), schistosomiasis infect 200 million people and is endemic in 76 tropical developing countries [5]. There are four type of Schistosoma cause infection in humans. S. haematobium, Schistosoma Mansoni, Schistosoma Japonicum, and Schistosoma Mekongi. S. haematobium is associated with bladder cancer. In general lives in the venules of the human urinary bladder. Eggs laid in the urinary bladder produce irritation and tissue fibrosis, that may cause to the development of bladder cancer [6]. Schistosomiasis is a parasitic infection that affects 200–250 million people in the world. The parasite enters the body via skin and joins portal circulation after maturation which takes up about 1–3 months. After that, it reaches venous plexus of bladder via rectal and inferior iliac vein. Schistosoma infections cause cancer by a different number of mechanisms. All changes induced by Schistosoma eggs such as fibrosis, hyperplasia and metaplastic chances are all precancerous changes [7]. Nitrosamine derivatives produced by chronic bacterial infections and their precursors found in urine are well-known bladder carcinogenic factors [8]. Infection and related urinary stasis caused by fibrosis increase endogenous carcinogens' concentration and intensify their carcinogenic effects on bladder epithelium [9] [10]. Increased miracidium and beta-glucuronidase enzyme levels, caused by mature Schistosoma infection, source the release of carcinogenic amines into the urine [11]. Most common genetic changes in bladder cancer is the loss of heterozygosity on chromosomes 9p and 9q, which is found regardless of tumor grade and stage [12]. Transurethral resection of tumor is the essential treatment in non-muscle invasive bladder cancer [13]. As we mentioned in our case, etiology of squamous cell bladder cancer includes Schistosoma haematobium infection too. Standard treatment modal for Schistosomiasis-related bladder cancers is radical cystectomy and urinary diversion. Efficacy of neoadjuvant and adjuvant radiotherapies and chemotherapy is low. Pure squamous cell carcinomas are always seen with chronic bladder irritation and infections. Mixed type urothelial carcinomas with squamous cell carcinoma areas are more frequent than pure squamous cell carcinomas. Most of those tumors have an invasive, fungal-like or infiltrative and ulcerative characteristic. True papillary structures are almost never seen. Cytological differentiation level changes from severe keratohyalin pearl formation to anaplastic giant cell tumors with a low squamous differentiation rate. It affects wide areas of the bladder and mostly deeply invasive at the time of diagnosis already [14]. Prognosis of these squamous cell carcinoma patients is usually bad. This is mainly due to the fact that the disease is already in a late stage at the time of diagnosis. In a study done by Richie et al. on 25 patient series, 5-year survival rate in patients with bilateral lymph node dissection and radical cystectomy was found to be 48% and the most important prognostic factor was reported to be tumor stage [15]. | ||||||
|
Conclusion
| ||||||
|
Squamous cell carcinomas, which are rarely seen in bladder tumors, can also be caused by Schistosoma infections. The young patients diagnosed squamous cell carcinoma cases who live in areas where this parasite infection is endemic, should also be reviewed for previous or current Schistosoma infections. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Ertugrul Gazi Ozbey – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Ertugrul Gazi Ozbey. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|